Laser Eye Surgery
From Only
£36/mo
Daily appointments available from the convenience of your own home.
Laser eye surgery is a type of treatment that corrects blurred vision to give you a life without glasses or contact lenses. It’s a rapid procedure which can be done in just a few minutes, and without any discomfort. For those undergoing SMILE and LASIK eye surgery the procedure is described as painless, for patients undergoing LASEK eye surgery they can expect some discomfort which should settle within a week or so.
Laser eye surgery can correct refractive conditions such as short-sightedness, long-sightedness, and astigmatism.
A state-of-the-art laser is used to reshape the cornea of the eye to give you clearer vision. Thanks to the latest advancement in technology, laser eye surgery is completely safe and the most popular elective surgery in the world.
Laser vision correction works by correcting the focus of the cornea. The different types of refractive eye surgery are: LASIK, LASEK, ReLEx SMILE, PRESBYOND. We are the only UK group to offer all these options, based on what is ideal for your unique vision correction needs.

At Optegra, we offer slightly different laser eye surgery procedures to reshape your cornea and correct the defects that affect the eye’s ability to see clearly
After you arrive at the hospital, our team will ensure you are comfortable and at ease prior to surgery. You can ask our specialist team any questions you have about the surgery or aftercare process while we explain the day’s procedure from start to finish.
Here are the surgical steps involved in LASIK (the most common laser eye surgery procedure):
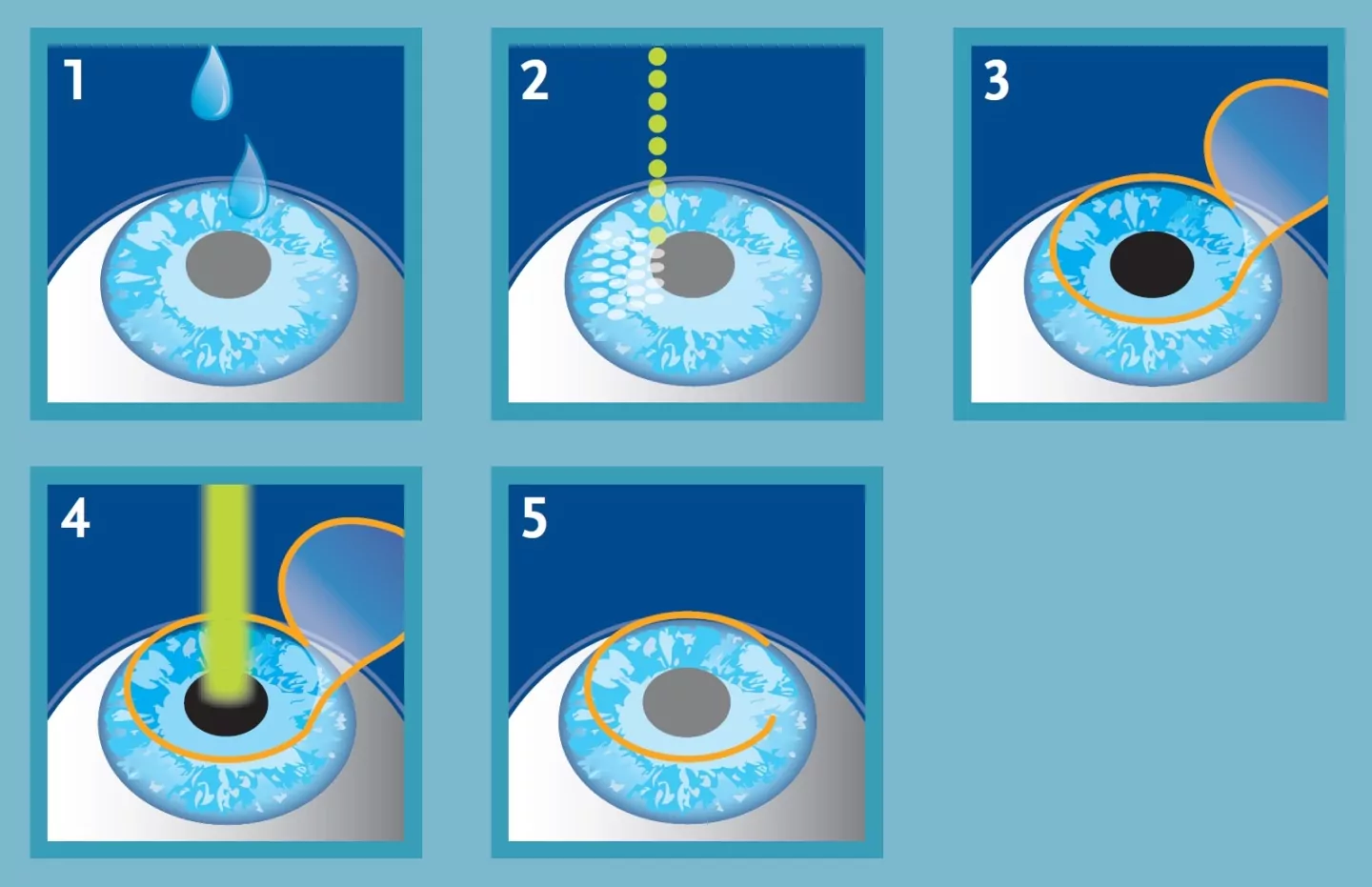
The technique used for SMILE is slightly different. No flap is created for SMILE procedures. Instead, SMILE uses a femtosecond laser to create a small, disc-shaped lenticule within the corneal tissue, which contains the portion of the cornea to be removed for vision correction.
The surgeon makes a tiny incision on the cornea to access the lenticule, which is then removed through this incision. The lenticule is carefully separated and removed, reshaping the cornea to correct the refractive error.
LASEK involves removing the outermost layer of the cornea, the epithelium, as a thin sheet or with the use of an alcohol solution. This layer is then temporarily set aside.
Similar to LASIK, an excimer laser is used to reshape the underlying corneal tissue.
After reshaping, the epithelial sheet or alcohol-treated epithelial layer is repositioned on the cornea’s surface and secured with a soft contact lens to protect and facilitate the healing of the epithelium.
LASEK typically involves a longer and sometimes slightly more uncomfortable recovery period compared to LASIK due to the need for the epithelium to regenerate and heal. Vision improvement may be more gradual.
Whichever procedure you have, if you think you may be anxious on the day, you can opt for a mild sedative to relax you.
After the surgery is complete, you’ll be able to relax in a comfortable recovery area. Eye drops and complete aftercare instructions will be provided. You can leave for home as soon as you’re comfortable. Your first aftercare appointment will be set up before you leave the hospital.
You will be able to see after your treatment, although your vision might be a little hazy.
While the treatment suitable for you will be determined according to your personal needs during our free initial consultation, we offer one clear set price for our laser eye surgery. We offer a range of helpful financing, including up to 24 months completely interest free. Our indicative price range is below:
Best suited for people with thin corneas and low-moderate prescriptions.
Can treat a wide range of prescriptions and popular for a fast recovery.
The most advanced method with fast recovery using well established keyhole technology.
Blended vision is ideal for age related near changes and helps people see far-middle-near.
Important Information:
Presbyond & Complex Laser are charged at £2,795 per eye. Interest free credit & finance options available.
Learn more about the cost of laser eye surgery

Laser eye surgery is ideal if you are affected by short sight, long sight or astigmatism. Short-sightedness can range from mild, where treatment may not be required, to severe, where objects will appear blurry.
In the long term, long-sightedness can significantly cause headaches and tiredness due to “over-focus” and lead to double vision. Depending on the seriousness of the problem contact lenses or glasses can be worn but some people may find it less of a hassle to have laser eye surgery.
While laser eye surgery is a safe and effective option for many individuals with refractive vision problems, it may not be suitable for everyone.
Factors that can make someone unsuitable for laser eye surgery include:
Age: Laser eye surgery is typically not recommended for individuals under the age of 21 because their eyes are still developing. On the other hand, it may not be ideal for people over the age of 40 who are experiencing age-related vision changes, as they may require reading glasses after surgery. There are alternative procedures, such as Presbyond, available for those over the age of 40.
Unstable Vision: Candidates should have stable vision for at least one to two years before undergoing laser eye surgery. Rapid changes in vision can make it challenging to determine the appropriate correction.
Certain Eye Conditions: Some eye conditions, such as keratoconus, severe dry eye, glaucoma, and retinal issues, can make laser surgery less suitable or even risky.
Pregnancy and Nursing: Hormonal changes during pregnancy and nursing can affect vision stability, making it advisable to wait until hormonal fluctuations have stabilised before considering laser eye surgery.
Autoimmune Disorders and Medications: Certain autoimmune disorders and medications that affect the immune system can impact the healing process and increase the risk of complications.
While all surgical procedures carry a very slight degree of risk, laser eye surgery is an extremely safe, common and effective procedure – with over 40 million patients worldwide who have had corrective eye surgery!

Awarded top-rated surgeon by Doctify in 2018
Optegra laser eye surgery is very safe and effective. Over 99% of our customers achieved 20/20 vision or better on the next day after the treatment although it may take slightly longer for some patients.

Our immaculate five star, dedicated hospitals provide the best possible setting for the very best care and outcomes for laser eye surgery. Our world class laser eye consultants are NHS-trained, as well as being Fellows of the Royal College of Ophthalmologists or equivalent organisations. Our ophthalmic surgeons are the best in the industry so you can rest assured of their experience and expertise.
With hospitals and clinics throughout the country, an Optegra Eye Hospital is never far away.
Aftercare is an extremely important part of our laser eye surgery treatment. Our well-rounded aftercare programme is designed to ensure that every patient gets back on their feet in no time at all. It starts right after the day of your laser eye surgery and is tailored to your individual needs. We will regularly check on your recovery to ensure that you get back on your feet in no time.
All Optegra patients have access to the professional advice of our team of fully NHS trained surgeons and staff to answer any of your questions on eye health or procedure
Optegra gave me the extra 5% I needed – and that made all the differenceJudd Trump
World #1 Snooker Champion
Optegra eye hospitals are dedicated only to laser eye surgery, eye treatments and eye care. Our services include laser eye surgery, lens replacement and cataract surgery and treatment for other medical eye conditions including glaucoma.
Our hospitals and clinics provide a modern, calm and comfortable environment in which our patients can feel relaxed and well cared for through a patient-led, personalised treatment plan.
As centres of eye excellence, we offer facilities with the most advanced surgical and technical equipment. Each location is staffed by a professional clinical team with leading NHS-trained consultant laser eye surgeons who are all Fellows of the Royal College of Ophthalmologists. The Medical Advisory Committee (MAC) at each hospital ensures compliance with the best clinical practice.
As well as purpose-built Optegra hospitals in Birmingham, Hampshire, London, North London, Manchester, Surrey and Yorkshire, we have conveniently located outreach eye clinics in Maidstone, Newcastle and Uttoxeter.
Laser eye surgery takes 15 minutes to perform, but the actual laser takes a very small part of this time. However, we would advise that you allocate 2-3 hours during the day for a correct preparation and initial aftercare steps to take place. At Optegra, we have invested in state-of-the-art advanced laser eye technology to ensure the best possible results for our patients, meaning our patients’ experience is quicker and more comfortable.
Most patients will see the results of laser eye surgery 1-2 days after their surgery. Since everyone is different, some patients enjoy a rapid visual recovery after laser eye surgery and can notice improvements in their vision immediately.
After a patient has had laser eye surgery, they can usually return to work within 24 hours after LASIK or SMILE laser eye treatment, and within a few days after LASEK laser eye treatment. However, every individual is different and it is important that all patients take as much time as they need to recover. Our laser eye surgeons, or a member of our team, will be on-hand to provide any advice or reassurance during the recovery period. In general, most patients are able to go back to work and drive after 48 hours.
Effectively, by reshaping the cornea, laser eye surgery will permanently correct a patient’s vision. LASIK, LASEK and SMILE Laser eye surgery treatments are considered a permanent cure for most refractive errors, however some patients may find they need reading glasses at a point in their lives as the eye naturally ages. This condition is also known as presbyopia.
While many people are apprehensive about pain during their laser eye surgery procedure, in reality, it is comfortable and pain-free. There is also very little discomfort felt following the procedure, so there is nothing to worry about if fear of pain is stopping you from having surgery.
Laser eye surgery is typically a quick procedure. The actual time will vary depending on the type of laser procedure you have opted for. SMILE and LASIK typically take 15 minutes per eye, while LASEK takes around 20 minutes per eye.
The three main types of laser eye surgery are LASIK, LASEK and ReLEx SMILE.
LASIK is the most popular type of laser eye surgery. A laser creates a flap which is gently lifted so the cornea can be reshaped. This treatment has a rapid visual recovery time for some patients.
LASEK is best suited for patients with less serious eye focusing problems, specifically patients with thin corneas or dry eyes who may not qualify to have LASIK. Instead of creating a flap, the fine surface of the cornea is loosened and folded back, then the cornea is reshaped.
ReLEx SMILE stands for Small Incision Lenticule Extraction, and is the least invasive laser eye treatment compared to LASIK and LASEK. There is no need to create a flap; instead the cornea is reshaped through a keyhole procedure which means some patients usually benefit from a short recovery period.
Yes. Our specialist Monovision technique can help correct reading vision difficulties caused by presbyopia. However, LASIK, LASEK or SMILE surgeries may not always be suitable for people who need strong prescriptions to read. In this case an alternative treatment may be suggested.
If you are unsure whether you are suitable for laser eye surgery, please don’t hesitate to get in touch to arrange a free, no-obligation consultation with one of our laser eye surgeons, and see how we can help you.
In short, the answer is yes. However, each case is unique, so your consultant will assess individual suitability to ensure that you are eligible for another treatment. Essentially, it will depend on the amount of tissue in the eye and how much of it was removed during the first surgery.
Each laser eye surgery treatment is suited to different individuals with different eye health needs. LASIK is best suited to patients with hyperopia or myopia, whereas LASEK is suitable for individuals with thin or flat corneas.
ReLEX SMILE is suitable for individuals with or without astigmatisms. At Optegra, we understand that everyone is different. During your free consultation with one of our expert laser eye surgeons, you will undergo an in-depth assessment to determine which laser eye treatment is best suited to you.
At Optegra, we do not perform laser eye surgery on anyone aged below 21. This is because the eyes are still developing during childhood and adolescence, and vision changes can occur during this period.
For older patients, it is not recommended to have laser eye surgery past the age of 40, as they might experience age-related vision changes imminently requiring them to wear glasses. For patients who are around 40, Presbyond is a unique laser treatment that could be more suitable.
Yes. In fact, laser eye surgery is a highly effective method for correcting astigmatism, along with other refractive errors like nearsightedness (myopia) and farsightedness (hyperopia).
Yes, we offer a variety of financing options including interest free for up to 24 months.
By Author: Amir Hamid
Mr. Amir Hamid is our Medical Director for Vision Correction and an expert refractive surgeon, based in London. Medically reviewed on: Thursday 28th September 2023.
Not ready for a consultation? Learn more about our range of treatments, doctors and hospitals
Information packBook your virtual consultation with our top rated eye hospitals
Book NowWe'll answer any questions you may have about treatment.
Private: Mon-Thu: 8am-7pm, Fri: 8am – 5.30pm NHS: Mon-Fri: 8am – 6pm
Manage your existing bookings & payments
Patient Portal