Diabetes is a lifelong condition that causes a person’s blood sugar level to become high and it can affect many parts of the body – including the eyes. In fact, it is estimated that 3.5 per cent of people with diabetes will be registered blind due to their diabetes.
Here, Optegra Eye Hospital Manchester consultant surgeon, Abha Gupta, and Optegra optometrist Nigel Burgess share their views on the details you need to know to help you protect your vision.
There are two types of diabetes:
- Type 1 – where the body’s immune system attacks and destroys the cells that produce insulin
- Type 2 (the most common) – where the body does not produce enough insulin
Fluctuating blood sugar levels can cause serious health problems if not treated, meaning people with the condition have to carefully control their diet and activity levels. Organs that can be damaged by diabetes include the heart, kidneys and eyes as well as feet and gums.
How can diabetes affect eyes?
Diabetes affects the eyes when your blood sugar level is too high, causing blood vessels in the retina to swell and leak.
In the short term you may not experience any loss of vision but you could experience:
- Blurry or wavy vision
- Frequently changing vision
- Dark areas or vision loss
- Poor colour vision
- Spots or dark strings (or floaters)
- Flashes of light
High blood sugar levels can also cause a number of eye conditions – and the key to preventing this is early detection.
Early detection is vital
Attending regular eye tests and screening is essential for diabetics so that any changes in the eye can be detected and treated quickly.
In the UK anyone over the age of 12 with diabetes is offered screening on an annual basis because:
- Diabetic retinopathy may not cause any symptoms in the early stages
- Screening can detect problems in the eyes before it affects your vision
- The condition if not diagnosed and treated promptly can lead to blindness
- If detected early, treatment can prevent or reduce the risk of vision loss
The screening programmes which were introduced in 2013 have shown a positive reduction in the number of people with more advanced retinopathy and registration of blindness.
How can regular eye tests reveal diabetes?
As part of a regular eye test, which all adults are recommended to have every two years, your optometrist will measure the eye pressure as part of the check for conditions such as glaucoma. They will also examine your eye using an ophthalmoscope to check the fine detail, as this can detect swelling at the back of the eye – a possible sign of diabetes.
Eye tests can also detect cataracts even at early stages and check for bleeds at the back of the eye due to high blood pressure or diabetes.
By having your eyes regularly checked, optometrists can see changes very early and sometimes start treatment before you notice any changes to the vision.
Eye conditions which can be caused by diabetes include:
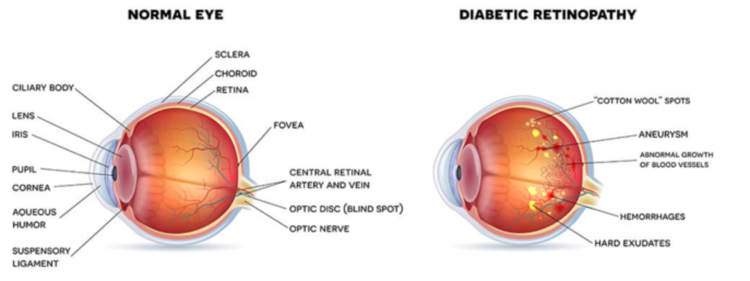
Diabetic retinopathy
If the blood glucose level stays high over time, it can cause damage to the tiny blood vessels in the retina, the back of the eye. These vessels, particularly if undiagnosed or untreated, can bleed and cause damage to the photoreceptor cells, which allow the retina to process light into images in the brain. This is called diabetic retinopathy or diabetic macular oedema.
Diabetic Macular Oedema
Diabetic macular oedema is where the central part of your vision that you use for your fine detail, such as reading, is affected by diabetes. Fluid or blood to collect within the retina causing a loss of sharp vision. If untreated this could progress and cause some loss of vision or blindness.
Cataracts and glaucoma
Cataracts can develop quickly for diabetics with poor glucose control and make your vision more blurred until it is quite difficult to see. Glaucoma can develop as a secondary condition particularly when someone already has diabetic retinopathy and is caused when nerve bundles in the eye are damaged resulting in a loss of peripheral vision.
Treatments for diabetic retinopathy
There are several ways to treat any changes noted at the back of the eye. A healthy lifestyle and good glucose control is key. Laser and injections are also common, although sometimes surgery may also be necessary.
The treatment for diabetic changes in the eye is rapidly progressing with newer injections which last longer in the eye and are more specific to the diabetic changes alone and have the potential to renew healthy vascular growth, reverse retinal degeneration. These may provide hope for the many who do not respond to current treatments.
More effective treatments are being developed with ultimately the need for less frequent hospital visits. Lasers are also being advanced to be more effective.
Living with diabetes
Lesley Schimell, age 83, has been treated at Optegra Eye Hospital Manchester. She says:
“I was diagnosed with Type 2 diabetes in 2002 at the age of 62. It was a shock as I had no family history of diabetes and I was not overweight. I followed the recommended regime for the next 15 years and had the usual podiatry checks for neuropathy and diabetic eye screening checks for retinopathy.
“In 2017 I had a CT scan for hypoparathyroidism and a tumour was found on my pituitary gland, which was exerting pressure on the optic nerve and would eventually cause blindness. A decision was taken to remove as much of the tumour as possible, and as a result my diabetes has reduced to acceptable levels most of the time.
“In 2020 I was referred by the diabetic screening service to the eye hospital as they had found that not only did I have cataracts on both eyes but that both eyes were affected by age related wet macular degeneration.
“I was referred to Optegra Eye Hospital where I now receive treatment for wet AMD by Intravitreal Injections every 6 weeks. My consultant has informed me that my sight has improved and I feel this also. I believe these visits and injections have saved my sight and I am very grateful for the care received. They sound scary but just like an injection anywhere you get used to it.”
Optegra is proud to offer the most advanced optical treatments available, including laser eye surgery, cataract surgery, and lens replacement. If you would like to speak to one of our expert ophthalmic surgeons, contact our team today.
