Glaucoma
Get Referred Today
For Free

Get Referred Today
For Free

For more information please leave your details below:
For more information please leave your details below:

Glaucoma is one of the leading causes of preventable sight loss in the UK.
At Optegra, we offer fast access to consultant-led glaucoma surgery and treatments through the NHS, using advanced techniques to reduce pressure in the eye and help protect your vision. Our glaucoma services are currently available at Manchester, Bradford and Nottingham Eye Hospitals, with North London and more locations launching soon.
Glaucoma is a group of eye disease where the optic nerve – which connects the eye to the brain – gradually becomes damaged. This is usually caused by a build-up of pressure inside the eye. Over time, this pressure can lead to permanent vision loss if left untreated.
Due to glaucoma developing slowly and with no early symptoms, many people don’t realise they have it until noticeable vision loss has occurred. It is one of the leading causes of irreversible sight loss in the UK, especially in people over 60.
There is currently no cure for glaucoma, but with early diagnosis and the correct treatment, further vision loss can often be prevented. At Optegra, our glaucoma specialists use the latest technology to detect and treat the condition effectively.
Twin and population studies have shown that having a close relative with glaucoma – particularly primary open-angle glaucoma (POAG) increases your risk of developing the condition. Individuals with a family history of POAG are 4 to 9 times more likely to develop it themselves
If you have a parent, sibling or grandparent with glaucoma and you are aged 40 or over, it’s especially important to have regular annual eye examinations. Detecting the condition early is the best way to slow its progression and reduce the risk of permanent vision loss.
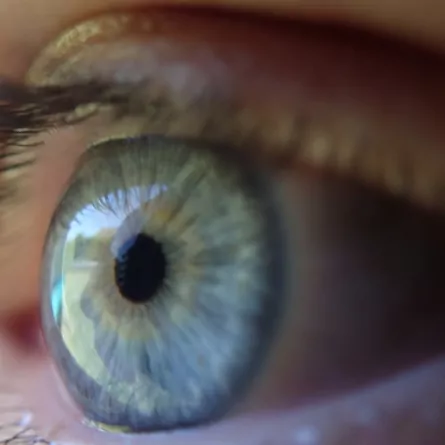
Our specialists will assess the type and stage of glaucoma before recommending the most suitable treatment plan. Types of glaucoma include:
The most common form, where drainage becomes less efficient over time, increases pressure inside the eye. Risk factors include; age POAG is more likely to affect people over 40, particularly those with a family history, West African ancestry, short-sightedness or diabetes.
Occurs when the drainage angle between the iris and cornea becomes blocked. It requires urgent treatment and is more common in women, particularly those who are long-sighted.
Secondary glaucoma occurs when increased eye pressure is caused by another underlying eye condition, injury, or surgical complication. It disrupts the eye’s normal fluid drainage, which can lead to optic nerve damage if not treated.
Pigment Dispersion Glaucoma – This type develops when pigment granules from the back of the iris break off and circulate within the eye. These granules can block the drainage system, leading to fluid build-up and raised intraocular pressure. It typically affects younger, short-sighted individuals and may not cause symptoms early on.
Pseudo-exfoliation Glaucoma (PXF) – A rarer form of glaucoma where abnormal protein-like material builds up on the lens and inside the eye. This material can clog drainage pathways, increasing eye pressure and leading to optic nerve damage. PXF is more common in older adults and can progress more rapidly than other types of glaucoma.
A rare form present from birth or early childhood, usually due to developmental abnormalities. Early treatment is vital to preserve vision.

Consultant ophthalmic surgeon and Glaucoma lead at Optegra
The treatment pathway can vary for glaucoma patients, from those whose condition is stable and low-risk and who are regularly monitored at their community optometrist, to those with more complex, high-risk cases who need surgical intervention or treatment at a Trust hospital. However, there is a large cohort of patients in the middle who need to be monitored by glaucoma specialists and this is where we at Optegra can help. With the new monitoring, review and treatment service, we will only need to refer those who need complex trabeculectomy surgery on to Trusts – which means speedier access to treatment, as well as helping relieve Trust waiting lists for glaucoma.

Glaucoma is one of the leading causes of blindness in the world. In the UK, it’s estimated that around 10% of people with glaucoma will experience significant sight loss. With an ageing population, the number of those affected is expected to increase, making early detection vital.
This is the most common form of glaucoma and develops gradually over time.
In its early stages, open-angle glaucoma typically doesn’t cause any pain or noticeable symptoms. Many individuals do not realise they have it until some vision has already been lost. They may report blurred vision or frequently bumping into objects. It usually starts by affecting peripheral (side) vision and can progress to affect central vision at end stages, if left untreated.
Risk factors include:
If you’re in any of these groups, regular eye checks are essential to detect changes early and begin treatment if needed.
This less common type of glaucoma can develop suddenly and is considered a medical emergency. When the drainage angle of the eye becomes blocked, pressure can rise rapidly and cause:
If you experience these symptoms, seek urgent care to prevent permanent vision damage.
The raised pressure in my eyes meant that I had blurred vision and dryness, and my eyes would often feel very tired. After moving to the UK, I went for an eye test and within two weeks I had an appointment at Optegra’s new glaucoma clinic in Manchester. My experience there has been brilliant – all the staff are friendly and patient. Dr Nihal is very professional and explained everything clearly, so I now have a thorough understanding of my condition. My treatment is ongoing – I started with laser, and I will go back in two months’ time for the results. The location is so convenient for me, and it means I don’t have to wait at the main NHS Trust hospital.
At Optegra, we offer the following NHS glaucoma treatments:
The iStent is a tiny implant placed in the eye during cataract surgery to help manage open-angle glaucoma. It improves fluid drainage within the eye, helping to reduce intraocular pressure.
This minimally invasive procedure is completed at the same time as cataract surgery and usually adds just a few minutes to the operation. Most patients can return to normal daily activities within a few days, and many find they need fewer glaucoma medications afterwards.
SLT is a quick, non-invasive laser procedure used to treat open-angle glaucoma. It works by targeting the eye’s drainage system to improve fluid outflow and lower intraocular pressure.
The treatment is carried out in our clinic as an outpatient procedure. Anaesthetic eye drops are used, and a special lens is placed on the eye to deliver the laser precisely where it is needed. The procedure typically takes around 5–10 minutes per eye, and most patients can return to normal activities shortly afterwards.
SLT can be particularly helpful for patients who are unable to tolerate eye drops or whose medication isn’t effectively controlling pressure. The effects can last for several years, and the treatment can be repeated if needed.
After your iStent or SLT procedure, our team will provide personalised aftercare and monitoring to ensure your eyes are healing well and that pressure is being effectively managed. Follow-up appointments are essential to track your progress and adjust your care if needed.
You’ll receive clear instructions on what to expect after surgery, what symptoms to monitor and when to return for review. Our team is always on hand if you have any questions or concerns.
When you come to Optegra for NHS glaucoma treatment, you’ll be in expert hands. Our surgeons are all NHS-trained, industry-recognised consultants and Fellows of the Royal College of Ophthalmologists.
Each procedure is carried out in one of our specialist eye hospitals and supported by highly trained clinical teams. From consultation through to surgery and aftercare, our focus is always on delivering the best possible outcomes for your vision.
Yes, many people with glaucoma can drive if their vision meets DVLA standards. Your optometrist or consultant can advise based on your specific case. However, you must inform the DVLA if you have glaucoma in both eyes, as it can significantly affect your vision.
Laser treatments like SLT can effectively manage glaucoma by lowering eye pressure, but they are not a cure. However, this condition requires ongoing monitoring.
Yes, particularly in cases of angle-closure glaucoma, which can cause intense eye pain or brow pain and headaches due to sudden pressure spikes.
Open-angle glaucoma typically progresses slowly over years, while angle-closure glaucoma can develop quickly and requires urgent care.
By Author: Robert Petrarca
Mr. Robert Petrarca is one of our Consultant Ophthalmologist and Ophthalmic Surgeons and an expert in glaucoma treatment, based in Maidstone. Medically reviewed on: Friday 11th April 2025.
Many thanks. We will be in touch shortly.